It looks like you are in the United States
We have a different site (www.q-bital.com) which better suits your location
The backlog of patients waiting more than six weeks for an endoscopy has increased substantially since the start of the Covid-19 pandemic, and waiting lists now need to be tackled as a matter of urgency. A recently published report by NHS England, calls for reform, and proposes introducing a network of diagnostic hubs in the community, some of which will contain endoscopy facilities.
A mobile or modular endoscopy unit can be used in the interim, or alongside a community hub, to create a stand-alone facility providing a distinct pathway for elective endoscopy services. An urgent need to address waiting times Endoscopy demand has grown substantially over the past five years, and although activity has increased, waiting times have increased more rapidly, causing a backlog. Flexible sigmoidoscopy procedures have seen the highest growth rates, largely due to the roll out of the bowelscope screening programme.
During Covid-19, the need to deep clean equipment and facilities between patients has led to a fall in productivity and cancelled procedures and, as a result, higher and longer waits. Overall, endoscopy activity levels reduced by over 90% at the peak of the pandemic.
Emergency endoscopic procedures at the peak of the pandemic were wherever possible undertaken in operating theatres with negative air pressure. Gastroscopy was also initially designated as an aerosol generating procedure (AGP), which carries a risk to endoscopists if patients are Covid-19 positive or Covid-19 uncertain, but gastroscopy is no longer considered an AGP under PHE guidance.
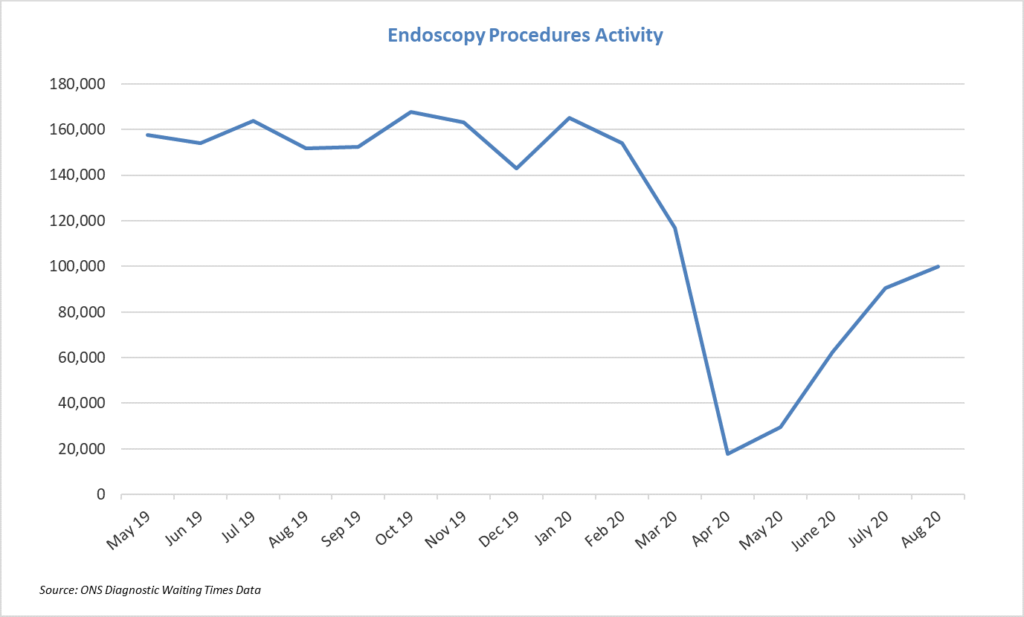 The most recent figures from NHS England shows that while endoscopy activity has increased substantially since April, the rate of recovery has slowed markedly. Activity in August was around two thirds of that in a normal month. This, in combination with the fact waiting lists have not increased substantially in August, despite the low level of activity, suggests that there is still a sizable ‘hidden’ backlog of people who have not yet made it onto waiting lists.
The need for future-proofing
There is now an urgent need to establish Covid-19 minimal endoscopy facilities to aid recovery. The report recognises that access to endoscopy equipment and facilities, in particular those for colonoscopy, were already under considerable strain before the pandemic. As well as workforce constraints, the Get it Right First Time (GIRFT) programme also revealed that around 20 NHS trusts are likely to require a complete rebuild of their endoscopy facilities with others needing improvement.
The most recent figures from NHS England shows that while endoscopy activity has increased substantially since April, the rate of recovery has slowed markedly. Activity in August was around two thirds of that in a normal month. This, in combination with the fact waiting lists have not increased substantially in August, despite the low level of activity, suggests that there is still a sizable ‘hidden’ backlog of people who have not yet made it onto waiting lists.
The need for future-proofing
There is now an urgent need to establish Covid-19 minimal endoscopy facilities to aid recovery. The report recognises that access to endoscopy equipment and facilities, in particular those for colonoscopy, were already under considerable strain before the pandemic. As well as workforce constraints, the Get it Right First Time (GIRFT) programme also revealed that around 20 NHS trusts are likely to require a complete rebuild of their endoscopy facilities with others needing improvement.
In the NHS England report, it is estimated that around 200 new endoscopy rooms are needed in NHS Trusts to cover current growth in endoscopy and enable the planned extensions to the bowel screening programme. New endoscopy decontamination units are also needed, and the report also recommends that all existing imaging equipment older than 10 years should be replaced.
Unfortunately, there is no national asset register for endoscopy facilities, and the report recommends equipment/facilities and staffing surveys should be undertaken urgently to facilitate both short- and longer-term planning. The report suggests participation in the National Endoscopy Database (NED) by the 20% of NHS Trusts that are not already doing so.
A report published by Public Policy Projects in partnership with Vanguard two years ago, showed that more than a third of hospitals are operating endoscopy decontamination suites with equipment approaching or exceeding manufacturers recommendations, and that around 25% of hospitals have endoscopy decontamination suites that are more than ten years old. A practical solution for endoscopy It is hoped that the establishment of Covid-free endoscopy facilities at some of the proposed diagnostic community hubs or one-stop-shops , along with testing of both patients and staff ahead of all procedures, can mean the requirement for deep cleaning between patients will be greatly reduced, allowing throughput to increase nearer to normal levels. Patients who are Covid-19 positive and those who need an emergency endoscopy before Covid-19 status can be determined should continue to have their procedures done in facilities with negative air pressure (usually operating theatres).
With regards to workforce, the report recommends the establishment of training academies to increase the amount of non-medical colonoscopists and to enable existing colonoscopists to take on screening colonoscopy. More endoscopy nurses will also be needed to meet additional demand.
Without investment or reformed service delivery, by its own admission the NHS risks being unable to meet targets, including the ambition to diagnose 75% of people with cancer at an early stage, and improving patient outcomes. Even if plans are swiftly approved, the recommendations in the report will take time to implement. But with the backlog growing each month, is waiting an option?
For each month productivity is compromised, the waiting list grows beyond a level that can be easily recovered without going above 100% of existing capacity. An interim solution is needed, and flexible clinical infrastructure could provide the answer. Mobile and modular endoscopy units can be combined with flexible endoscopy contamination units and set up in almost any location – adjacent to a diagnostic hub or elsewhere in the community - to create a stand-alone, Covid-free site for elective endoscopy.
Read the report, which includes a detailed review of endoscopy activity, here .
A copy of the report ‘Looking within: The State of Endoscopy in England’ , produced by Public Policy Projects in partnership with Vanguard, can be requested by contacting us .



Vanguard Healthcare Solutions
Unit 1144 Regent Court, The Square, Gloucester Business Park, Gloucester, GL3 4AD

We have a different site (www.q-bital.com) which better suits your location