It looks like you are in the United States
We have a different site (www.q-bital.com) which better suits your location
This week, alongside an oral evidence session held by the Health and Social Care Committee (HSCC) as part of their inquiry into the backlog in NHS waiting times, the Prime Minister announced the “biggest catch-up programme in NHS history”. Whilst funding to support substantive action to combat the elective care crisis is essential, it is important that resource is used to increase the resilience of health services against future crises, such as through investment in capacity-expanding infrastructure such as Community Diagnostic Hubs (CDHs) and surgical hubs.
The announcement detailed the government’s plans to invest £12 billion a year for the next 3 years across the NHS and social care sectors, naming the elective care crisis as a priority to solve. The newly released funding will be used to expand hospital capacity up to 110 percent, enabling 9 million more appointments, scans, and operations to be held, and will allow for the government’s ambitious targets of treating 30 percent more elective care patients by 2023/2024 compared to pre-pandemic levels, to be met. Furthermore, a portion of this sum is expected to be used as a capital investment into CDHs. Alongside this, Parliament heard from the Chancellor of the Exchequer who detailed the government’s existing commitments to expanding the healthcare workforce by delivering 50,000 more nurses and 50 million more primary care appointments to address the backlog.
According to estimations from Anita Charlesworth, Director of Research and Economics at the Health Foundation, it would take £17 billion for the government to reduce waiting times to the 18-week standard by 2024/2025. Charlesworth detailed these figures to the HSCC on Tuesday 7th September, noting that this approximation accounts for the pressures of a 12.5 million-long waiting list as patients continue to come forward after not seeking treatment during the pandemic. The newly announced funding excellently positions the UK to meet this target and sets the nation on a promising trajectory to tackle the backlog.
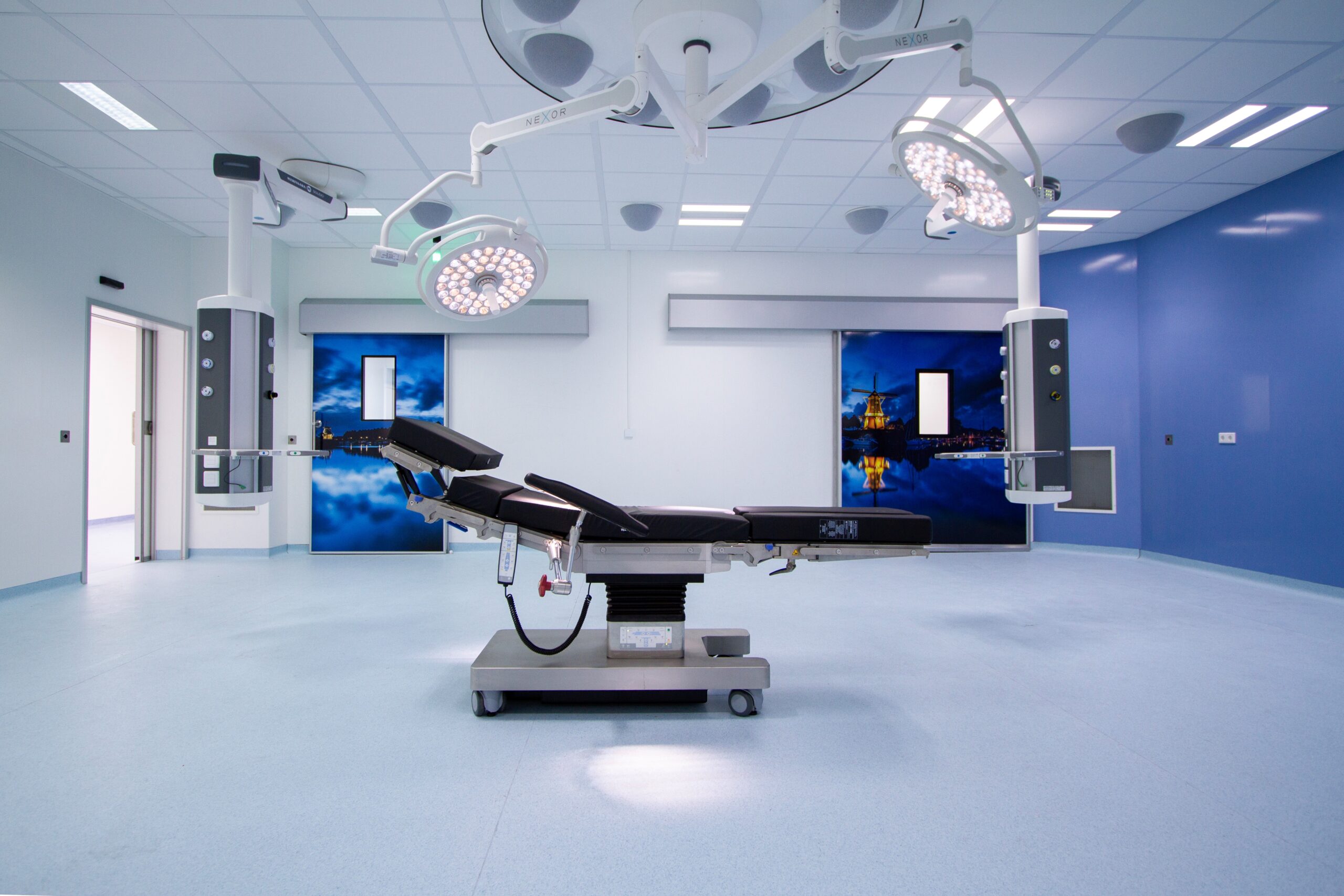
Also providing evidence to the HSCC during its inquiry was Professor Neil Mortenson, President of The Royal College of Surgeons of England (RCSE), who promoted the establishment of surgical hubs as a possible solution to this crisis. Previously, the RCSE called on the government to agree a ‘New Deal for Surgery’ that detailed 12 recommendations, including the proliferation of surgical hubs across the country, and a five-year government commitment to annual investments of £1bn for surgeries as the health service continues to tackle the compounded consequences of the pandemic and the backlog. The RCSE support the view that the construction of standalone surgical hubs, such as the facility built by Vanguard at Queen Mary’s Hospital in Roehampton, would better prepare surgeries for high-pressure situations, such as potential pandemics, and allow them to continue planned operations safely.
From the evidence given during the HSCC’s inquiry to the statistics discussed by the Prime Minister during his speech to Parliament, it is clear that tackling the elective care crisis is a matter of urgency and the ability to respond flexibly to the ever-changing needs of the community is of primary concern. The unique pressures that face the NHS require unique solutions. Vanguard’s bespoke modular facilities are primed to offer such solutions and act as “one stop shops”, supporting hospitals with a range of services in one location and reducing the pressure on them.
The modern methods of construction used by Vanguard allow for our hubs to be delivered substantially quicker than traditional brick and mortar facilities, with the site at Queen Mary’s Hospital being delivered in just 4 months. The establishment of standalone surgical hubs and CDHs across the country would transform the provision of healthcare in the UK, dramatically increasing capacity, and delivering revolutionary solutions to the elective care crisis.
To quote Dr Goddard during the HSCC’s inquiry, we must “never waste a good crisis”. Lessons must be learnt from the record-breaking backlog in elective care and bold improvements made to the current system to ensure that improved patient outcomes are prioritised. The establishment of CDHs and surgical hubs across the UK is this lesson - and the government cannot learn it quick enough.


Vanguard Healthcare Solutions
Unit 1144 Regent Court, The Square, Gloucester Business Park, Gloucester, GL3 4AD

We have a different site (www.q-bital.com) which better suits your location