It looks like you are in the United States
We have a different site (www.q-bital.com) which better suits your location
As the number of Covid-19 cases fall, hospitals and GP surgeries have begun preparing to resume routine appointments and planned procedures, such as elective surgery, endoscopy, diagnostic tests and scans. However, things remain a long way from ‘business as usual’.
While the most immediate crisis may be over, many hospitals continue to care for a large number of Covid-19 patients, with reports stating around 25% of intensive care unit beds need to be retained for this purpose. There is also a real prospect of a second wave, which – according to a number of experts, including England's chief medical officer, Professor Chris Whitty – has the potential to be even more deadly than the first.
At the same time, the waiting lists for elective procedures are increasing and are likely to continue to build even when planned surgery is reintroduced, since many hospitals won’t safely be able to immediately return to the same activity level as before the crisis. Some reports suggest that waiting lists for elective procedures could top 10 million by the end of this year. As a result, hospitals are under increasing pressure to resume this type of care as soon as possible.
The very term ‘elective procedures’ is increasingly misleading. It implies that patients have a choice of whether or not to go ahead with an operation. The reality is that many of those patients will be experiencing increasingly chronic pain and impairment to their lives, and the majority will not consider their procedure a choice, but an increasing necessity.
A key challenge hospitals are now facing in preparing to resume elective care, is how to keep both patients and staff safe from the risks associated with exposure to Covid-19, in particular given the fact that many of the patients requiring surgery or treatment are more vulnerable to illness because of other health conditions. There is also the risk that patients or visitors from outside will bring the virus into clean zones of the hospital, as could clinicians who need to travel between sites.
Access to tests for staff and patients prior to procedures taking place will be important, but the long turnaround times currently experienced for analysing tests could further add to waiting times and risk surgery being cancelled if the results are not back on time.
Managing the pressure on physical space can also be difficult, as there will be a need to maintain safe social distancing in clinical areas. In many cases, hospital facilities have been repurposed or redesigned to deal with the crisis, and internal space may be divided up into ‘Green’ and ‘Red’ zones, which will need to remain fixed for some time yet. This, coupled with the increased time required to change PPE, and to undertake full cleaning of procedure rooms between operations, will significantly reduce productivity in those hospitals that do restart elective procedures.
Many hospitals will have sufficient clinicians and staff to return to pre-COVID levels of activity, but with the reduced productivity will be unable to do so without additional physical capacity. Where will this additional capacity come from, and how will the patient journey for elective surgery impact on existing staff and patient flows?
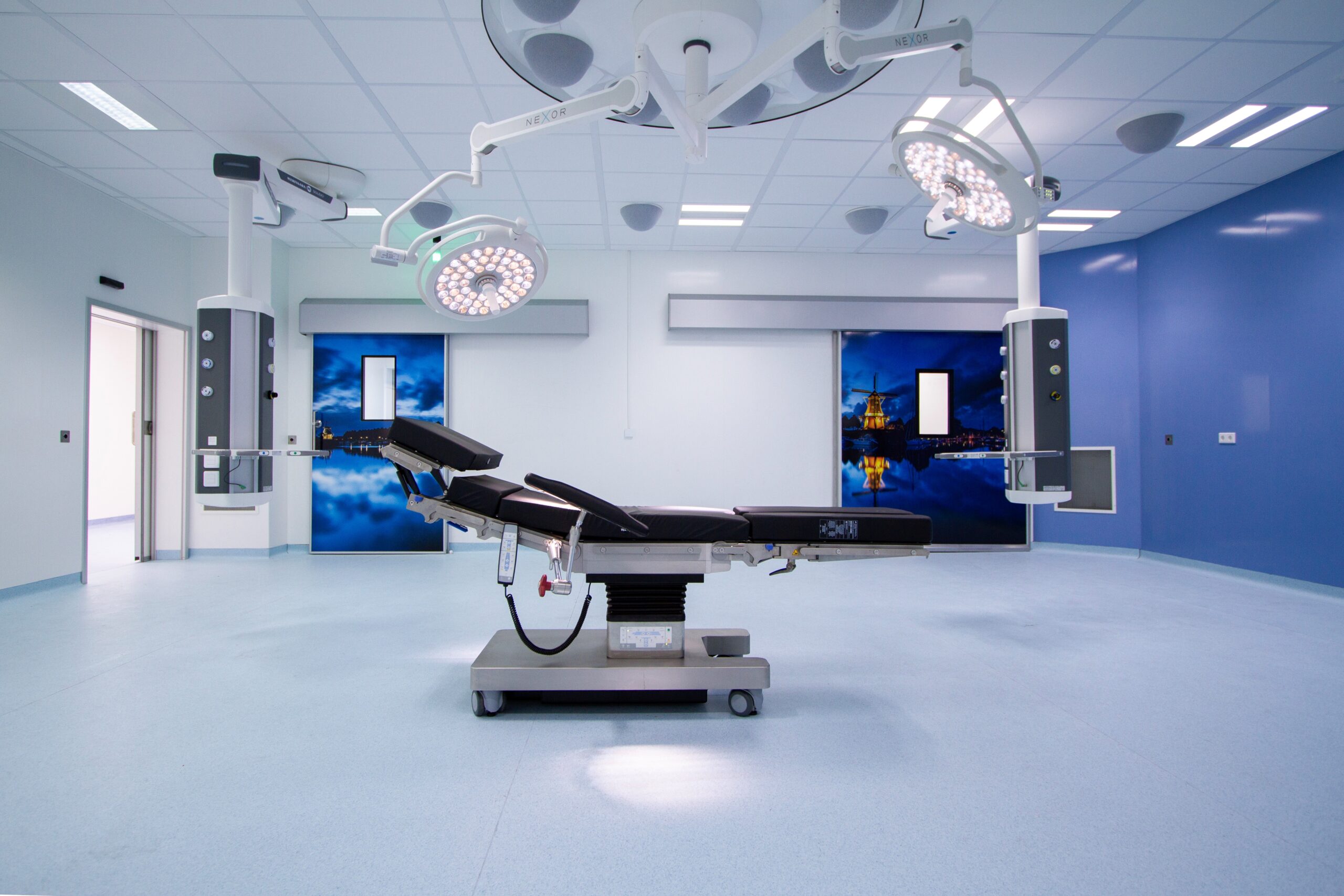
One potential solution could be to look at flexible healthcare infrastructure options. A mobile operating theatre could upscale hospitals’ Green zones by providing a safe space away from Covid-19 Red zones within the hospital itself. Combined with a mobile or modular ward, which could also house staff areas, this could provide a complete stand-alone Green zone where procedures can be undertaken safely, without putting additional pressure on other parts of the hospital.
Dr Hans Kluge, who is director for the WHO European region, said recently in an interview with The Daily Telegraph that now is the "time for preparation, not celebration". He stressed that, though the number of cases of Covid-19 in countries such as the UK, France and Italy was beginning to fall, it did not mean the pandemic was coming to an end, and that countries should use this time to start to build capacity in hospitals, primary care and intensive care units.
Since the pandemic and the resulting backlogs have brought a need for temporary additional capacity, it makes sense to consider flexible healthcare options that allow hospitals to upscale based on their needs. Mobile and modular facilities can be used either on a temporary or semi-permanent basis, as required.
Vanguard Healthcare Solutions provides temporary facilities to support healthcare providers when additional capacity is needed to cut waiting lists, to decant an existing theatre or in response to a crisis situation, and has been a trusted partner to the NHS for over 20 years.


Vanguard Healthcare Solutions
Unit 1144 Regent Court, The Square, Gloucester Business Park, Gloucester, GL3 4AD

We have a different site (www.q-bital.com) which better suits your location